Oncologic radiotherapy
Radiotherapy is an essential tool in the treatment of a large number of tumors. Radiotherapists are therefore an integral part of all multidisciplinary groups at the King Albert II Institute of the Cliniques Universitaires Saint-Luc.
They play an active role in the treatment of cancers, alongside surgeons and oncologists specialized in chemotherapy. They can define precisely the benefit of the irradiation techniques in each case discussed during the multidisciplinary meetings.
Radiation therapy, alone or in combination with other treatment modalities, is able to cure many tumors. In other cases, it aims to control certain symptoms of the disease, such as pain, but also to improve the patient’s quality of life.
What is radiotherapy?
The principle of radiotherapy is to irradiate cancer cells with X-rays. These cells, which already display numerous mutations due to their malignant nature, do not easily survive radiation. Radiotherapy is delivered in small daily doses that are tolerable for normal cells but gradually destroy the cancerous cells. This fractionated delivery of radiation has made it possible to considerably decrease the frequency and intensity of adverse effects. This technique is the most precise and well tolerated. Most of the time, it is performed on an outpatient basis and does no longer require hospitalization.
There are two types of radiotherapy:
-
Brachytherapy, or interstitial radiotherapy
In some cases, especially when the volume of the tumor to be treated is small, a specific irradiation technique is used. This method is called brachytherapy, or curietherapy, after the name of Marie Curie who discovered radium at the end of the 19th century.
Depending on the area to be treated, either small radioactive seeds are injected or thin radioactive plates are inserted. They then remain in contact with the tumor and deliver a slow radiation. The application takes place under general anesthesia, and, if necessary, under highly sophisticated ultrasound guidance that enables to see the organ in three dimensions. Dose calculations (dosimetry) are carried out during the implantation, thus allowing making the modifications that appear necessary at any time.
In our center, brachytherapy is performed for four kinds of tumors: eye melanoma (and some other tumors), breast cancer, skin cancer, and prostate cancer. Another field of application is the treatment of recurrent keloids (abnormal scars), but this is outside the field of oncology.
-
Conventional radiotherapy or external radiotherapy
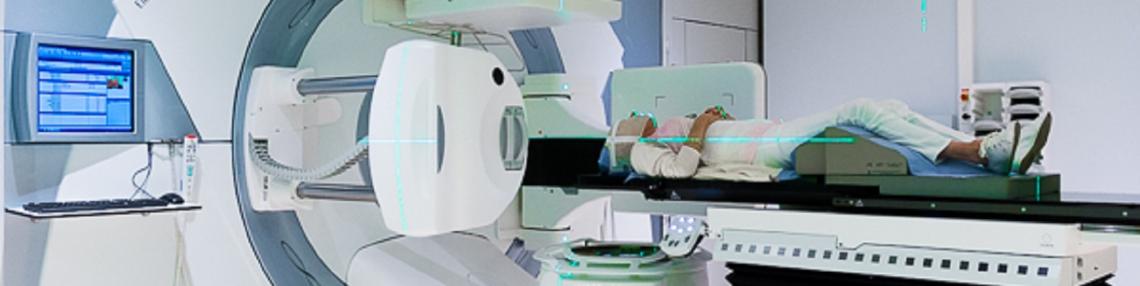
This is the radiotherapy technique that is most often used to treat cancer. It consists in irradiating the tumor using linear accelerators.
Our radiotherapy department is equipped with three linear accelerators, including the Ethos, from Varian, recently acquired by our center, offers for the first time in Belgium an adaptive therapy thanks to artificial intelligence!
What is the purpose of radiotherapy?
Radiotherapy is an essential tool in the treatment of a large number of tumors. This method can cure many tumors, alone or in combination with other therapeutic modalities. In other cases, it is used to control certain symptoms of the disease, such as pain, and to improve quality of life.
Type of care
In principle, there is no need to hospitalize you during radiation treatment. Hospitalization is, however, possible if you live far away, as well as if you receive concurrent chemotherapy or if your situation requires it. We will discuss and agree with you on the most appropriate means of transportation for your situation.
Should you use your own vehicle, you will benefit from a contribution from your health complementary insurance. In other cases, you can be transported by cab or ambulance, every day or several times a week. The choice of transportation depends on your health status. If you have any questions on this subject, you can contact the social service.
Duration
The total treatment duration can vary from one day to seven weeks. The duration is adapted to the evolution of your disease and also depends on how you tolerate the procedure. Do not worry if the specialists decide to change the duration of your treatment. They may also decide to carry out a new simulation during the course of treatment. They will also explain the reasons for this. The schedule you are given at the beginning of your treatment is essential both to you and to the team that takes care of you. Changing this schedule is not advisable. Should any unforeseen problems arise, please inform your doctor as soon as possible. Avoiding interruptions during your treatment as much as possible is crucial. A scheduled interruption must be agreed upon with your radio-oncologist. On the other hand, it happens that a radiation machine breaks down, causing the treatment to be interrupted briefly. We estimate that an interruption of no more than 4 to 5 days has no effect on the effectiveness of the treatment, but this varies greatly depending on the type of tumor treated. Do not hesitate to ask your doctor for information about this.
How to prepare for it?
Simulation is the first step of the treatment. The preparation is done with the help of a "simulator". This device allows us to locate and delimit with precision the part of the body that needs to be treated. The markings are drawn on your skin with a specific fuchsin-based red dye; small tattoo dots can sometimes be used.
A MRI or PET/CT scan is often necessary to determine, with more precision, the area to be treated.
During this examination, extremely precise images are taken of the targeted area, in the same position as the one during your treatment. This examination usually takes place during a separate appointment. A second simulation will be scheduled 7-10 days later to confirm the landmarks taken on the skin before starting the treatment. Simulation is essential to the proper execution of the treatment. It usually takes from 30 minutes to 1 hour, which can sometimes seem long. You will always be informed if a simulation is not necessary for particular reasons or if we use certain accessories during the simulation. Afterwards, your treatment will begin rather quickly under the supervision of the radio-oncologist. Data collected during the simulation are analyzed by computers. The radio-oncologist and the radiophysicist determine together the modalities of your treatment, such as the distribution of the radiation doses, the size of the fields to be irradiated, their number, and their orientation in space. Then, they check on the computer whether the treatment modalities are suitable for your personal situation.
As part of an adaptive radiation therapy using the Ethos system, the radiation ballistics is adapted for each of your radiation therapy sessions, according to the changes in your anatomy. This allows for more precise radiation therapy in certain circumstances. It is particularly indicated in tumors of the pelvis and abdomen, where changes in the shape and size of the bladder, bowel, and rectum are common. Your radio-oncologist will judge whether or not this technology is suitable for your disease.
Procedure
Before the first consultation, your medical file will have already been discussed and analyzed in a multidisciplinary meeting attended by your radio-oncologist. If not, your data will have been transmitted to the radio-oncologist so that he or she will have the necessary elements to determine the choice of your treatment, in agreement with your attending physician and the other specialists treating you. The radio-oncologist will ask you about your health problems and those of your immediate family in order to discuss the most appropriate treatment with you. He or she will also ask you about your life habits. If you agree on the treatment principle, the doctor will then explain it to you in detail.
For this type of treatment, you do not have to fast. The position on the treatment table will be identical to the one you had on the simulator table, usually laying on your back, sometimes on your stomach or side. The part of the body which will be irradiated will have to be stripped of all clothing. If some areas of the body are in the radiation beam and should not be treated, they will be protected. On some devices, the protection of these body parts is ensured by metal blocks placed on a tray; in this way, they are not directly on the body but between the device and the patient.
You must not move during the irradiation to prevent a part of the body that is not meant to be treated to be irradiated. However, you can only continue to breathe calmly. During the irradiation, the beam is directed very precisely on the targeted part. The machines rotate and make noise. You can still communicate with the treatment team via a microphone, even if you are alone in the treatment room. The team will look after you through two video cameras. Irradiation only lasts a few minutes per radiation field, for a total of approximately 15 minutes per day. You do not become radioactive after the radiation session.
During the course of your treatment, you can always make an appointment with one of the radio-oncologists. This is also a good opportunity to ask questions. The treatment has sometimes to be adapted to your personal situation. A different machine than the one with which you started your treatment with may be used.
The radio-oncologist will determine which examinations and medications may be needed during treatment.
What happens after treatment?
You may be offered other treatments after radiation. The radio-oncologist, in consultation with the referring physician and other specialists, will examine you regularly to assess your situation.
Inconveniences
You may have to wait your turn for a radiation session or consultation. We make every effort to minimize waiting times. Delays are usually due to equipment adjustments, an emergency situation, difficulties with another patient's placement, or a request for information from another doctor about a patient. The team in charge of your treatment will strive to explain the reasons for the waiting time. Do not hesitate to ask for an explanation, especially if you do not understand how appointments are arranged.
Adverse effects
As for any treatment, radiotherapy can cause adverse effects. They are very variable from one patient to another. They depend on the dose of radiation delivered, the part of the body treated, and the reactions of each patient. They gradually diminish in the weeks following treatment cessation. Many patients experience few or no adverse effects. It goes without saying that the treatment of these adverse effects will be adapted to your complaints and difficulties. The doctor will inform you about the potential adverse effects and suggest the most appropriate treatment for your condition. Reporting any reaction to both the health care team and the doctor is of utmost importance. Fatigue is normal and will go away little by little.
Fatigue
Rest regularly, take short walks and exercise lightly. Take caloric and protein supplements, vitamins, and trace elements.
Headaches
Ask for prescription of a medication by the radio-oncologist.
Diarrhea
Ask for prescription of medication by the radio-oncologist and adopt a low-residue diet.
Decreased appetite
Eat small amounts more frequently. If you wish, you can seek advice from a dietician.
Anxiety and depression
Talk about it, you can improve your condition by getting help from a psychologist, by establishing a contact with other patients and friends, and also by using appropriate medication, if needed.
Skin irritation, itching
Never use any product without asking your doctor. The radio-oncologist can prescribe appropriate ointments and local care.
Hair loss
Irradiation of a hairy area, such as scalp, beard, pubic hair, armpit, etc., may cause hair loss. The hair will usually grow back within a month, depending on the dose of radiation delivered. Hair loss can also be caused by certain chemotherapy treatments.
Mucosal inflammation
Medications can be prescribed by the radio-oncologist.
Cystitis
Drink abundantly; specific medication can be prescribed by the radio-oncologist.
Answers to your questions
I have to wait for a long time before starting my treatment. Why?
In some cases (after surgery), it is advisable to delay the start of treatment to allow for proper healing.
Do I have to stop working?
By law, you are entitled to full work incapacity. The effects of radiotherapy can vary significantly from person to person. Some people feel better when they continue working full-time or at least part-time. Your employer may also adjust your working hours.
Can I stop my treatment?
This is not advisable and must only occur in agreement with your doctor.
I feel tired. Why?
Fatigue is not only due to the radiation, it can also be related to stress and sleep disorders. It can be a sign of depression as well. The advice given to you will depend on the cause: in case of sleep disorders avoid naps, in case of depression try not to sleep longer than usual. In general, it is better to exercise than to rest more than usual. During radiotherapy, your body consumes a lot of energy. The feeling of tiredness or weakness will slowly decrease after the end of the treatment. In order to limit the feeling of fatigue after treatment, it is best to avoid excessive efforts; you can also try to sleep longer, and if possible, take a short nap.
How can I prevent nausea?
You can ask your doctor to prescribe a suitable medication to you. Having a light meal before radiation may sometimes help.
Should I follow a diet or avoid certain foods?
Your diet should be varied and balanced. In certain circumstances, you may be asked to adapt your eating habits. You should eat slowly and avoid fatty, spicy, acidic, alcoholic, or very hot food. It is best to eat frequently, but in small amounts. You can seek advice from the radio-oncologist and a dietician if needed.
What to do in case of appetite loss?
To cope with the disease, your body needs extra calories. Minimal physical activity can stimulate your appetite. Eat what you are drawn to and in small quantities but frequently. Should you need help, do not hesitate to talk to your doctor or a dietitian.
Do I have to continue my treatment for high blood pressure, cholesterol, and diabetes?
You will be asked about the medications you are taking by the radio-oncologist during the first consultation. He or she will decide if changing your treatment is necessary. Usually, there is no need to interrupt the treatment prescribed by your treating physician or specialist. If there is any problem, the radio-oncologist and your treating physician will discuss an appropriate solution.
How should I dress?
You can dress as usual. Tight-fitting clothes or synthetic fabrics might irritate the skin. We thus recommend that you wear loose cotton clothing. Remember that during the treatment, your clothes may be stained by the dyes used on your skin to draw the treatment landmarks.
Is there any special care for the skin?
This depends on the targeted body part. A particular cream or ointment may be prescribed if needed. We also usually advise the use of mild cosmetic products without detergents.
Does treatment change sexual behavior?
Many patients experience changes in their sexual desire and intercourses during treatment. If you have any difficulties, do not hesitate to talk about it to the competent staff. When irradiating a woman's pelvis, we usually advise to avoid sexual intercourses during and immediately after the treatment. Irritation of the mucosa might cause painful intercourse.
Can radiotherapy make you infertile?
Radiation targeted on the pelvis can cause temporary or permanent infertility. Cessation of menstruation and appearance of other typical signs of menopause should generally be expected. Specific treatments can be proposed. In men, irradiation of the sexual organs reduces sperm production and their ability to fertilize. If you wish to have children and are concerned that the treatment may make you sterile, preserving frozen sperm before starting the treatment is possible. In the same way, it is also possible to store frozen eggs for women.
I am also undergoing chemotherapy. Why?
Radiotherapy is only a localized treatment. It only acts in the irradiated area. Chemotherapy acts on the whole body and prevents malignant cells from spreading. If chemotherapy is prescribed, it can be started before, during, or after radiation. The doses of each treatment can be adjusted as needed if both are started at the same time.
I have been called for an examination a few weeks after the end of my treatment. Why?
The medical follow-up does not stop with the end of radiotherapy. We analyze the results and evaluate any reactions to the treatment. We also initiate additional treatments if necessary. Special examinations (X-rays, blood tests, etc.) may be necessary and are done in collaboration with the other doctors treating you.
Can I go on vacation?
Yes, as long as the radiotherapy is finished. Your attending physician or radio-oncologist will inform you of the precautions to be taken. If necessary, they can contact a doctor who lives in the vicinity of your holiday destination. If you plan to go to a sunny place, you should avoid exposing the treated body part to the sun, especially during the first year following the irradiation. When travelling abroad, we can only advise you to inquire about the coverage by your complementary health insurance or by the insurance companies, etc.
This sheet refers to a brochure of the SFRO (French Society of Radiotherapy-Oncology).
The ABRO (Belgian Association of Radiotherapy-Oncology) thanks the SFRO for allowing the use of this information.
Innovation and expertise
Irradiation techniques have progressed substantially in recent years. The contribution of information technology makes it possible to locate the tumor and determine its position with a very high precision. Massively irradiating the cancer while preserving the surrounding healthy tissue is now possible. The computer revolution is far from over. It will undoubtedly lead to further advances in the use of radiation.
Our center’s experience in defining the space occupied by a tumor in the body and its characteristics, such as shape, extension, location in relation to neighboring vessels, etc., is internationally recognized. Advances in imaging are fully exploited in order to optimize the way radiation therapy is delivered. This is made possible thanks to the close collaboration between experts in imaging, radiotherapy, and anatomy. The research unit of the radiotherapy department devotes a significant part of its activity to imaging techniques applied to radiotherapy.
The irradiation of cancers is becoming more and more precise. Massive doses are delivered to the lesion while the surrounding healthy tissue is spared.
The modern linear accelerators that equip our department use the most precise irradiation techniques currently available.
Advances in imaging allow us to optimize the way radiation is delivered. Our Ethos accelerator is equipped with a high quality on-board scanner that identifies the anatomical changes that occur during each treatment session. Using artificial intelligence, the treatment is then automatically adapted to the patient's new anatomy to improve treatment accuracy. This highly innovative adaptive therapy is certainly the future of radiotherapy.
In total, the radiotherapy department is composed of nearly 40 people. This also includes medical physicists, who are as numerous as the doctors. Their role is to constantly check for proper functioning of the state-of-the-art tools, to verify the calibration of the measuring instruments, etc.
This perfectly illustrates the major attention given to the quality control of the care: the irradiation techniques become indeed more and more complex and require increasingly sophisticated devices.
Irradiation is carried out according to an extremely strict procedure. It is first simulated on the screen. Then, subsequent checks are made to ensure that the patient's irradiation is fully in accordance with the data calculated during the preparation phase. These very drastic verification procedures prevent accidents.
The competence of the King Albert II Institute's radiotherapy experts in the field of quality control is internationally renowned. It translates into the development and publication of quality assurance programs that serve as a reference.
Radiotherapy oncology consultation secretariat
+32 2 764 47 52
Floor:
-4
Road:
986
